Loading...
Loading...

4 mins read
A study by Michigan Medicine reveals that obstructive sleep apnea, a common but underdiagnosed respiratory disorder, could increase the risk of dementia, especially in women. The results highlight the importance of detecting and treating this condition to protect long-term cognitive and cardiovascular health.
A prevalent sleep disorder that often remains undiagnosed may play a role in the onset of dementia in adults, especially women, as revealed by a Michigan Medicine study. The researchers arrived at this conclusion by analyzing survey data and cognitive assessments from over 18,500 adults, assessing the impact of obstructive sleep apnea, whether diagnosed or suspected, on dementia risk.
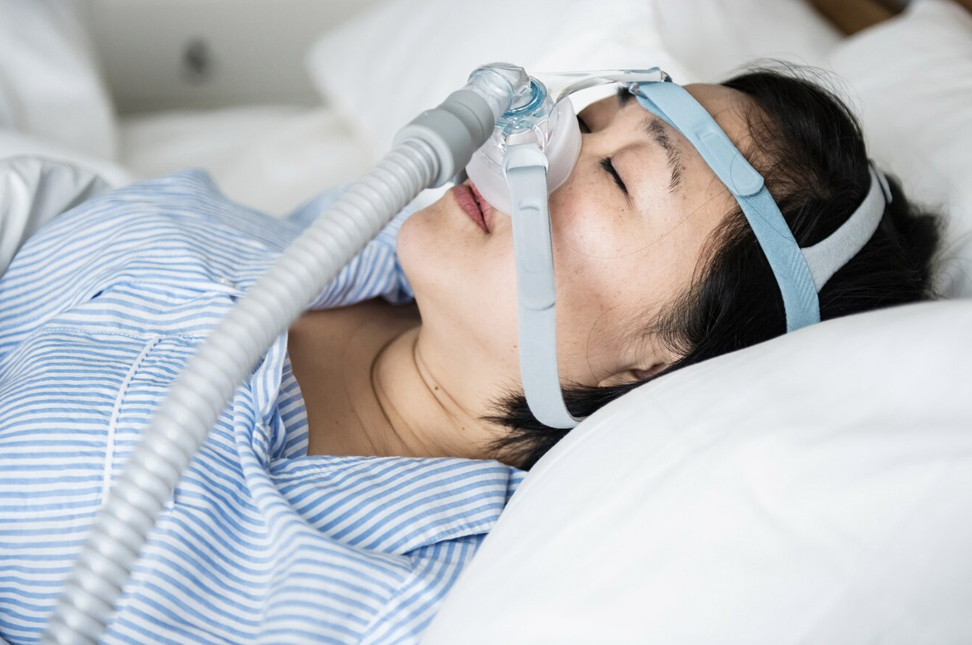
Obstructive sleep apnea is a chronic condition marked by episodes of interrupted or restricted breathing during sleep. For adults over 50, having obstructive sleep apnea, whether diagnosed or with evident symptoms—since many people are unaware of their condition—is associated with a higher likelihood of showing signs or receiving a diagnosis of dementia in subsequent years. Although the overall difference in dementia diagnoses did not exceed 5%, the association was statistically significant, even after adjusting for other factors that could influence the risk of dementia, such as race and education. At any age, women with diagnosed or suspected sleep apnea had a higher likelihood than men of being diagnosed with dementia. In fact, the rate of dementia diagnoses decreased in men, while it increased in women with age.
These findings offer a new perspective on the role of a treatable sleep disorder in long-term cognitive health, both in men and women. Although the reasons behind the differences in dementia diagnoses according to sleep apnea between sexes are not yet fully understood, researchers propose several possible explanations. Women with moderate to severe apnea could have a higher risk of cardiovascular diseases and are more prone to experiencing insomnia, factors that can negatively affect cognitive function. The decrease in estrogen during the transition to menopause also impacts the brain. During this period, women are more likely to face memory problems, sleep disturbances, and mood changes, which can contribute to cognitive decline. Although sleep apnea tends to increase significantly after menopause, it often goes undiagnosed. More epidemiological studies are needed to better understand how sleep disorders affect women's cognitive health.
Even though sleep is not considered an official risk factor, the commission indicated that sleep apnea "could be associated with dementia" and recommended including dementia screening questions for people with this disorder. Other modifiable risk factors, such as cardiovascular diseases and mental health problems, could also be aggravated by untreated sleep apnea. These potential adverse effects of sleep apnea, which can compromise performance and cognitive health, highlight the importance of early diagnosis and treatment. Obstructive sleep apnea, along with the sleep deprivation and fragmentation it causes, is also associated with inflammatory changes in the brain that could contribute to cognitive decline.
The Michigan Medicine study utilized existing data from the Health and Retirement Study, a continuous survey representative of Americans aged 50 and older. This study design cannot conclusively prove that sleep apnea causes dementia, so a long-term randomized trial would likely be needed to compare the effects of treating apnea with the effects of not treating it. However, since it could take a long time, or such a trial may never be conducted, retrospective analyses like the one conducted by the researchers, using large databases, may be among the most informative for years. Meanwhile, the results provide new evidence that both doctors and patients should consider when making decisions about the diagnosis and treatment of sleep apnea, considering the possibility that untreated apnea may cause or worsen dementia.
In Chile, approximately half of the adults in the Metropolitan Region suffer from sleep respiratory disorders, with 16.2% of these cases being moderate to severe. These disorders are more common in men, especially between the ages of 40 and 60, while the incidence in women increases significantly after menopause. The clinical manifestations of sleep apnea vary between sexes, which can delay diagnosis in women and limit their access to treatment, negatively impacting their quality of life and raising their cardiovascular risk. In sleep clinics, the ratio of men to women treated is approximately 7 to 1, attributed to differences in risk factors and clinical manifestations related to this condition (Saldías et al., 2017).
Despite being common, this sleep disorder often goes undiagnosed, which can have long-term negative consequences on cognitive health. These findings underscore the need for greater awareness of sleep apnea and the importance of timely diagnosis and treatment to mitigate its impact on the mental and physical health of those affected. Considering sleep apnea as a potential risk factor for dementia is crucial in the search for more effective approaches to preserving cognitive health in the population.
Sources